Sitting on a classroom chair, my body shaking, my head bouncing, is the first public seizure I can recall. It was kindergarten and my five-year-old classmates continued on with their work as if nothing was happening. They were used to it. But for me it was my first vivid memory of hydrocephalus. It is a condition that continues today, Now that I am a university student, studying journalism, I can mostly control the condition, but there are occasions when my fellow students have witnessed my seizures.
Hydrocephalus is a lifelong condition that affects two out of every 1000 infants. I am one of them.
It’s a condition, most diagnosed in early childhood and for me, it presented when I was just five months old.
Hydrocephalus affects the flow of cerebral brain fluid on the ventricles, causing deformities such as head enlargement and can also inflict epileptic seizures. The early signs of pre-diagnoses in infants from newborn to the age of five can vary for each patient, the most common are seizures and infections such as chicken pox and meningitis. When an infant is born, if there is a developing notice of hydrocephalus the head will enlarge with the parts where the skull hasn’t formed yet, growing further away.
My mother Rebekah Vidler recalls how the diagnosis impacted the family.
“In the beginning there was a lot of heartbreak,” she says. “There wasn’t a lot of information available back them. Not a lot of support.”
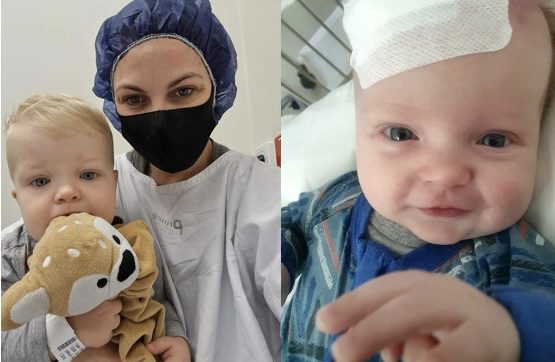
Mother Kerryn Csik describes the mix emotions within the family when her son Henry was diagnosed at eight months. Henry is now three.
“I was in a lot of denial, obviously we didn’t know what it was, so we really had no idea what was going on,” Ms Csik explains.
“When the doctor came in and told us, he essentially said to us they had no real further knowledge about it.
“They sent us to Brisbane. He didn’t even tell us about the cyst, we found out about that on the flight to Brisbane by overhearing him.
“It’s really difficult knowing that you have a helpless baby with a lifelong condition that you can’t do anything about.
“You know that he’s going to be in for brain surgery, that he’s going to be having multiple times in his life and it’s just really hard not knowing how to support him properly.”
Hydrocephalus is not rare, although many have still not heard of the condition. When a child is diagnosed, for many parents there is shock and confusion.
Jacob Wales, was diagnosed as a teenager at the age of 16, reveals his uncertainty at the health care system in the United States.
“After 13 years I feel that I have been lucky, that my upbringing and the privileges that has helped fund my survival due to this horrible chore; (but) I do feel that the system has let down so many Hydrocephalus sufferers in this country,” he says.
The only major way of managing Hydrocephalus is by implanting a device called a shunt. They vary from model and manufacturer; some are standard, and others can be programmable. In Australian there is a shunt registry, which was started by the Hydrocephalus Support Association, in collaboration with specialists. The president of the HSA Andrew Garde explains that the registry looks for trends in the data.
“There are just over 5,000 records, so we are just about to start doing some deeper research because there’s enough data to do some more population longitudinal research,” he says.
“We can start doing now some other things that we’re looking at being at to add to the registry of patient-reported outcome measurements.”
However, shunt failures occur 50 per cent of the time within the first three years of a diagnosed child’s life. The main cause is device infection. There are different models of shunts made by manufacturers who specialise in certain models. Shunts are mainly implanted in four different parts of the brain, either front left or right and rear left or right. The most common shunt model is the ventriculoperitoneal shunt that was developed and manufactured by Cogman. Many neurosurgeons have certain preferences regarding hhunt models, With VP shunts being the one of choice for most surgeons.
During pregnancy education and testing for neurological defects the condition has improved over the years, although if a child has been diagnosed after birth there are still stages of improving the survivability of the infant before they are fit for surgery and shunt implementation.
“Since the nineties there has been improving tactics for a child’s survival before shunt implantation, even before birth women are encouraged to take supplements during pregnancy as well as regular check-ups to battle the chance of diagnose,” Mr Garde says.
To verify a shunt fault such as an infection or blockage, scans are needed, including an MRI or CT. Further scans might be required and take place in a nuclear medicine clinic. During a shunt study, the specialist injects a small amount of contrast dye into the shunt reservoir to check the flow of CSF. If there is a blockage it is shown by a pause in the flow of the dye moving down from the shunt reservoir to which part of the body the catheter ends.
The other strategy to detect shunt failures is a procedure called shunt tapping, this implementation can also be strategised to remove CSF and remove pressure on the brain.
Developing countries have some of the highest statistics of infant deaths due to hydrocephalus. the high rate of childbirth in countries such as India contributes to the poor access to neurosurgeons and treatment for hydrocephalus sufferers in rural communities in these countries.
Infants with Hydrocephalus and their parents often have to travel long distances to get treatment in capital cities. Poorer countries, for example nations in Western Africa, require support from charities and NGOs for emergency clinical support and surgery. In less developed countries, there is more risk of infant deaths related to Hydrocephalus. Fever, infections and leaving neurosurgical care too late can all contribute to death.
There are charities such as Mercy Ships that have the facilities to perform advanced surgeries such as head reconstruction and shunt implantation. The only fault is that they can only travel to a country that has a port, therefore a child with Hydrocephalus in Central Africa for example will have to travel to countries such as Liberia or Guinea on the West African coast. Putting the geographical issues of medical care aside, funding in many poorer countries for hydrocephalus research is much less than in nations such as The United States, Australia, or the United Kingdom. Funding for universities to research Hydrocephalus and its effect on young children is much less than the funding that is available for diseases such as childhood cancer.
Mrs Vidler gives advice to parents if their child is diagnosed with Hydrocephalus.
“Seek medical attention, read up on research, join support groups and seek emotional support for yourself,” she says.
In the past twenty years, there have been large strides in raising awareness of Hydrocephalus and its effect on the patients who suffer from it.
Many people tell me I am brave for going through so many brain surgeries.
Hydrocephalus sufferers do not want to be washed down with sympathy. That is the reason behind the backward step. What’s needed is more awareness.
I have lived with Hydrocephalus for almost 24 years, but I think it’s in the recent months that the condition has gained me the most strength.